The First Seven Days: Establishing Breastfeeding in the Critical Hours Following Your Birth
The first week after birth is one of the most important windows in your breastfeeding journey. It is a time of deep learning, body-to-body connection, and incredible physiological change for both you and your baby. If you are wondering, “How do I get breastfeeding off to the best start?” or “Is it supposed to hurt this much?”, you are not alone. These first seven days are powerful, but they can also be overwhelming. This blog will guide you gently through them.

The Golden Hour and the Magic of Colostrum
Why That First Feed Matters
The first hour after birth is known as the “golden hour.” During this time, uninterrupted skin-to-skin contact helps regulate your baby’s temperature, heart rate, and breathing. Most importantly, it triggers their instinct to root, latch, and feed. Colostrum, the thick, golden first milk, begins to flow during this time. I am of the personal opinion that the Golden Hour should be renamed as the Golden Day, as the longer skin-to-skin occurs for, the better the outcome for breastfeeding.
What Makes Colostrum So Special?
Colostrum is rich in immunoglobulin A (IgA), leukocytes, lactoferrin, and growth factors that coat your baby’s gut and build lifelong immunity. It also acts as a natural laxative, helping to clear meconium and reduce the risk of jaundice (Ballard & Morrow, 2013). It is low in volume and calories, but densely packed with everything your newborn needs in the early hours and days. In short, colostrum is perfectly engineered by design to provide your baby with 100% of their immediate nutritional needs after birth.
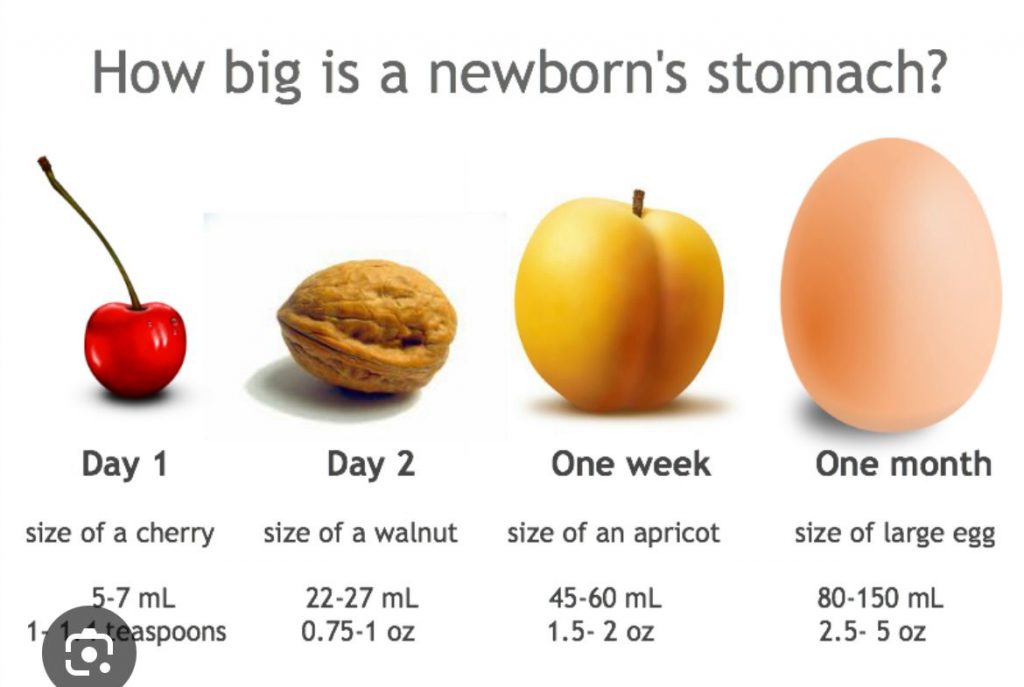
This small volume is by design. Your baby’s stomach at birth is about the size of a cherry and therefore they cannot take on even a tablespoon of liquid at any one time. Frequent feeding is vital to draw the colostrum through, keeping your baby’s tummy full and to encourage your milk to mature… all whilst soothing and regulating your baby. Moreover, your baby has received 24/7 nutrition from you in the womb, so they won’t be ‘starving’ within the first hour or two following the birth.
What Happens If You Had Interventions During Your Birth?
C-section, Epidurals and Opiates
Babies born via caesarean or medicated birth may be sleepier in the first 24 hours. Opiates used in epidurals can cross the placenta, affecting a baby’s alertness and feeding reflexes (Torvaldsen et al., 2006). In these cases, early skin-to-skin, gentle breast compressions to mimic a baby stimulating the breast, and responsive feeding are vital. Try hand expressing colostrum if baby is too sleepy to latch, it is also a perfect way to manage glucose levels. There is also evidence that due to the omission of baby travelling through the birth canal, latching can take a little more work to perfect.
IV Fluids and Swollen Areola
Large volumes of IV fluid during labour can cause swelling in your breast tissue which is a possibility if you had a long labour with a drip for the duration. This makes latching more difficult, especially if the areola becomes too puffy or taut for your baby to grasp effectively. You can use reverse pressure softening, a technique that gently shifts fluid away from the nipple area using your fingers before attempting a latch (Cotterman, 2004). Consequently, you may need a little help from your birth partner to keep baby close to you whilst you use both hands to do this.
Birth via Forceps and Suction (Ventouse)
If you had an instrumental birth, depending on the method and expertise of the medical professional, you baby may experience jaw tension, bruising, or even mild misalignment in your baby’s head or jaw, making their latch more challenging. If your baby seems unable to open wide or struggles to stay latched, a feeding assessment is essential. A qualified lactation consultant or breastfeeding counsellor can help identify tongue or jaw issues and suggest techniques like exaggerated latch and bodywork referrals.
A competent newborn osteopath is your first port of call when it comes to assessing and gently correcting misalignment. During an appointment, the osteopath can assess and correct any issues with your baby’s palate, head, neck and shoulder tension, reflexes and rebalancing. To find a newborn osteopath near you, you can Google ‘newborn osteopath X area’ or ‘cranial osteopathy X area’.
How to Achieve a Perfect, Deep Latch: Understanding a Good Latch
Next, a deep latch is the cornerstone of comfortable, effective breastfeeding. So how can you achieve this?
Firstly, your baby’s chin should come into contact with your breast first and press in snugly, with your nipple resting on baby’s philtrum to stimulate a wide open mouth. Secondly, bring baby to the breast (don’t move towards baby) and check for a flanged bottom lip, that baby has a double chin. More of the lower areola should be in the mouth, and you should be able to see some of the top of your areola above baby’s top lip. Next, both cheeks should be equally in contact with your breast, and baby should be looking ahead over your breast. Finally, baby’s nose should be clear of your breast, gently resting above.
If you feel you need to try and re-latch, you can pop a clean pinky finger in the side of babe’s mouth to release the latch. Take a moment to get comfortable and try again. Once you are happy (or happier!) with the latch, hold baby nice and snugly to you so that they feel stable and supported. You should hear steady swallowing, although it can be subtle in the first 24 hours due to the low volume of colostrum.
It is common to need several attempts at first. That is okay. Reposition, breathe, and try again.
Feeding Positions that Work for all Birth Recoveries
For vaginal births, a laid-back position supports your baby’s reflexive movements. For caesarean recovery and if you had an episiotomy, the rugby hold or side-lying can protect your incision or cut. Always bring your baby to your breast, not the other way around, to prevent strain and poor latch.
Troubleshooting Early Challenges: “Why Do My Nipples Hurt?”
It is normal for nipples to feel tender in the first few days. Your nipple is slightly elastic and is being drawn toward the soft palate during a feed. This can feel intense at first. Pain that continues beyond the first minutes of feeding, or visible damage like cracking or blistering, means the latch needs adjusting.
If you are one of the 20% of women Raynaud’s syndrome, you may experience vasospasm in your nipples which can feel like a sharp pinch. Your nipples will go white temporarily and feel cold to the touch. Don’t panic – this scenario usually gets better within the first few weeks. Gentle, warm heat pads can help alleviate, but don’t shock your skin by applying very hot water due to the risk of chilblains.
Use deep breathing or box breathing to stay calm through initial discomfort. Re-latching with better positioning usually brings relief within seconds.
Coping with Nipple Pain
- Let breasts air-dry after feeding.
- Use cooling gel pads or warm compresses between feeds
- Apply a small amount of expressed milk to aid healing
- Avoid soaps, drying creams and moisturisers – especially when the nipple is cracked or there is visible skin sores.
- Seek professional support to correct the latch
Your nipples and areola need to be kept free of artificial (and most natural) ointments, creams and moisturisers. Not only do the Montgomery glands on your areola secrete a form of lubrication to protect the nipple and areola, but you don’t want your baby to be consuming or coming into contact with harsh chemicals.
The Case for Exclusive Breastfeeding From Birth: Why Formula Top-Ups Can Set You Back
Babies are born wanting to feed often. That frequent feeding is designed to signal your breasts to increase milk production. Offering formula in the early days, even when well-meaning, can interfere with that feedback loop. If baby’s stomach is full of artificial milk, they may not cue to breastfeed, which slows your milk coming in. It can also upset your baby’s gut microbiome, which stabilises through frequent ingestion of your colostrum and mature milk.
Instead of topping up, offer the breast again. If baby is too sleepy or struggling, hand express and feed via syringe or spoon. Harvested colostrum from pregnancy can be useful, but your fresh milk is best. No pump will stimulate your breasts as well as a baby or hand expressing in these early hours.
If you’re reading this newly postpartum and had a midwife or consultant facilitate a formula top-up, don’t panic. Feeding your baby breastmilk going forward will help to rebalance their microbiome, and feeding on demand will help to regulate your supply.
Engorgement and the Milk “Coming In”: Welcome to the Day Four Boob Job
Many women wake up on day three or four looking like they have had a breast augmentation. This is milk transition time, and it is very exciting! You’ve done an amazing job with the held of your baby. However, your breasts may feel hot, tight, or lumpy. So, what do we do about it?
This engorgement is temporary. Feeding frequently and effectively, massaging while baby feeds, and using reverse pressure softening before feeds can ease discomfort and improve latching. Avoid tight bras and consider cool compresses after feeding.
Breastmilk Composition
Mature milk is made up of around 87% water, 7% lactose, 4% fat and 1% protein (Ballard & Morrow, 2013). It is also packed with hormones, enzymes, stem cells, and antibodies that continue to support your baby’s immune system for years to come. As a result, your milk is perfect for your baby, and contains exactly the right amounts of nutrients to support their growth and brain development.
Feeding Twins or Tandem Feeding From Birth
Tandem feeding is possible and beautiful. Whether you are feeding a newborn alongside a toddler, or twin newborns, your body can produce milk tailored to both children’s needs. Many mothers of twins go on to breastfeed exclusively.
Kathryn Stagg IBCLC offers brilliant support through her dedicated Twins and Triplets Breastfeeding Group here , which is a fantastic resource to bookmark. You can also check out the Association of Breastfeeding Mothers advice here on tandem feeding here.
Birth Recovery and Self-Care in the Early Days
Healing from Birth
If you had a caesarean, episiotomy, or tear, your body needs rest to recover. Breastfeeding while reclined or side-lying is not only effective, it allows you to rest deeply and prevent stitches from snagging or being pulled. Get help lifting baby or use pillows to support your arms and back. Every time you feed, you are also promoting uterine healing and helping your womb contract.
Emotional Recovery
Tears can be uncomfortable. Exhaustion can feel overwhelming. The first few days are intense. Ultimately, you will need to find a rhythm that suits you in terms of healing and going about your days, but this should be with some outside help. Therefore, if you are able to pull in support, whether it’s a weekly cleaner, a friend or your mum to help cook food or help with older children, or hiring a postnatal doula, your recovery will feel smoother.
Similarly, breastfeeding triggers the release of oxytocin which can make you sleepy, happy and restful. To help set yourself up for a positive recovery period, make up a ‘breastfeeding basket’ that travels around the house with you. Snacks, water, magazines, breast pads, the TV remote, phone charger and a baby changing bag for nappies, wipes and bibs, can all live in there to be at arms reach when needed. Your partner can get into the habit of topping it up for you.
Finally, you will be unlikely to book a birth reflections with your hospital for the first few months after birth, and the waiting time can be quite long for an appointment. If you feel you need a birth debrief to air your thoughts and talk through your experience, request an appointment as early as your Trust allows. Alternatively, you can also book a debrief with an independant midwife or a doula trained to do so (like me!).
Fuel, Fluids, and Nourishment for Birth Recovery
Eat to Heal
Breastfeeding requires an extra 300–500 calories per day. Prioritise warming, nutrient-dense foods like oats, soups, eggs, root vegetables, and fatty fish. Include collagen-rich broths and iron-rich leafy greens to aid tissue repair. SMASH (Salmon, Mackerel, Anchovies, Sardines and Herring) are the perfect fish for postnatal recovery. The First Forty Days is a fantastic book rich in nutrient dense recipes to boost your healing.
You may feel like you are craving sugar, which is natural because your body needs more energy. It’s best to avoid sugary food as this can also hamper your milk supply. Instead, pasta, potato, sourdough, gnocci and beans are fantastic at keeping you full and feeding you with the vitamins and minerals needed for energy.
Snack every time you feed and keep a water bottle with electrolytes nearby, as you’ll have a little depletion from feeding so often. Likewise, dehydration can impact supply and mood, so it’s best so sip little and often (this will also help you have the dreaded first bowel movement). Eating well helps you feel stronger, steadier, and more like yourself again.
You’ve Got This, And I’ve Got You
Breastfeeding is natural, but it is also learned. In those first seven days, you will be recovering, bonding, feeding constantly, and riding an emotional wave. You are doing something powerful, and you are giving your baby the best start to life possible. If there is anything you do today – celebrate your body, celebrate you, and celebrate how far you’ve already come. You’ve birthed your baby, and now you’re nourishing them, all with your body. What an amazing achievment.
If you are feeling unsure or feel you would like a one to one breastfeeding support session, please know that support can make all the difference. Whether you are pregnant and wanting to prepare, or you have just given birth and want guidance, I am currently taking on new breastfeeding clients alongside my birth and postnatal doula practice.
Get in touch today to book a one-to-one session, ask your burning questions, and feel more confident in your feeding journey. You do not have to figure this out alone.
References:
- Ballard, O., & Morrow, A. L. (2013). Human Milk Composition: Nutrients and Bioactive Factors. Clinics in Perinatology, 40(1), 1–26. https://www.sciencedirect.com/science/article/abs/pii/S0095510812001352?via%3Dihub
- Cotterman, K. J. (2004). Reverse Pressure Softening: A Simple Tool to Prepare Areola for Latch. Journal of Human Lactation, 20(2), 227–230. https://pubmed.ncbi.nlm.nih.gov/15117523/
- Torvaldsen, S., Roberts, C. L., Simpson, J. M., Thompson, J. F., & Ellwood, D. A. (2006). Influence of Epidural Analgesia on Breastfeeding. BJOG, 113(6), 623–628. https://obgyn.onlinelibrary.wiley.com/doi/10.1111/j.1471-0528.2006.00934.x
- Unicef UK Baby Friendly Initiative. (2020). A call to action: Improving support for breastfeeding. https://www.unicef.org.uk/babyfriendly/